|

by Makia Freeman
June 30, 2016
from
Freedom-Articles Website
Spanish version
|
Makia Freeman is
the editor of alternative news / independent media site The
Freedom Articles and senior researcher at ToolsForFreedom.com (FaceBook here),
writing on many aspects of truth and freedom, from
exposing aspects of the worldwide conspiracy to
suggesting solutions for how humanity can create a new
system of peace and abundance. |
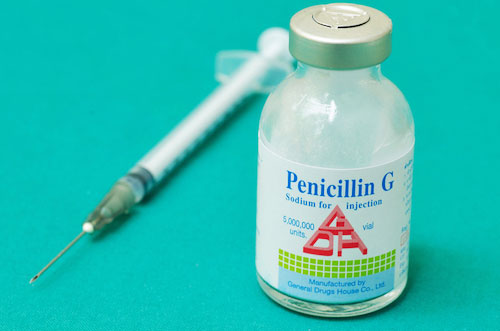
Antibiotic-resistant bacteria (superbugs)
have become a grave
problem due to
Western Rockefeller Medicine & Big Pharma
pumping the world
full of antibiotics like penicillin,
but now there may be
a natural solution:
the cannabis plant.
Antibiotic-resistant bacteria have become an out-of-control problem
in our world, as doctors and leading health officials know too well.
For over 100 years, Western
Rockefeller Medicine and
Big Pharma have been conjoined
twins attached at the hip; you cannot have one without the other.
Western medicine has fully embraced the drugs, radiation and surgery
model, and ever since the invention of drugs like penicillin
and methicillin, it has been throwing synthetic chemicals at
its patients to "cure" them.
Every action has an equal and opposite
reaction, and meanwhile, Life itself has found a way to
counterbalance the effect of
antibiotics overuse in the form of
antibiotic-resistant bacteria.
Some such as,
-
MRSA (Methicillin-Resistant
Staphylococcus Aureus)
-
MDR TB (Multidrug-Resistant
Mycobacterium Tuberculosis)
-
CRE (Carbapenem-Resistant
Enterobacteriaceae),
...are especially virulent
superbugs against which
Western Medicine has no defense.
The reason for this situation, of
course, is that antibiotics are like the proverbial sledgehammer or
cannonball to the mosquito, and by wiping out the human body's
entire bacterial presence in a certain area, you are wiping out the
beneficial bacteria which keep the harmful ones in check.
Our body literally depends upon this
bacterial balance as the foundation of immunity and health.
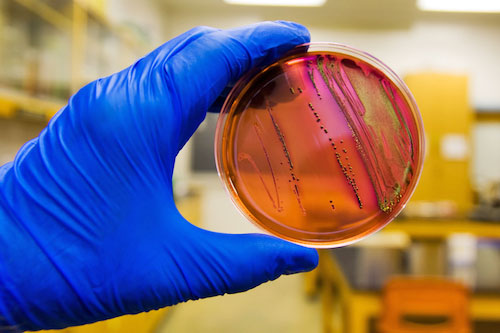
Antibiotic-Resistant Bacteria a
Grave Problem Across the World
Recent reports have highlighted the
massive problem.
This quote is from a report entitled "State
of the World's Antibiotics, 2015" by CCDEP (Center for Disease
Dynamics, Economics & Policy), a US-India health research
organization:
"Now,
however, once-treatable infections are becoming difficult to
cure, raising costs to healthcare facilities, and patient
mortality is rising, with costs to both individuals and society.
Decreasing antibiotic effectiveness has risen from being a minor
problem to a broad threat, regardless of a country's income or
the sophistication of its healthcare system."
"The
U.S. Centers for Disease Control and Prevention (CDC) estimates
that antibiotic resistance is responsible for more than 2
million infections and 23,000 deaths each year in the United
States, at a direct cost of $20 billion and additional
productivity losses of $35 billion (CDC 2013).
In
Europe, an estimated 25,000 deaths are attributable to
antibiotic-resistant infections, costing €1.5 billion annually
in direct and indirect costs (EMA and ECDC 2009).
Although reliable estimates of economic losses in the developing
world are not available, it is estimated that 58,000 neonatal
sepsis deaths are attributable to drug- resistant infections in
India alone (Laxminarayan et al. 2013).
Studies from Tanzania and Mozambique indicate that resistant
infections result in increased mortality in neonates and
children under five (Kayange et al. 2010; Roca et al. 2008)."
The WHO (World Health Organization),
despite being part of
the Rockefeller UN (United Nations),
acknowledges the massive problem in its
October 2015 fact sheet:
"Antibiotic resistance is rising to dangerously high levels in
all parts of the world. New resistance mechanisms emerge and
spread globally every day, threatening our ability to treat
common infectious diseases.
A
growing list of infections - such as pneumonia, tuberculosis,
blood poisoning and gonorrhea - are becoming harder, and
sometimes impossible, to treat as antibiotics become less
effective."
Dr. Keiji Fukuda, the Assistant
Director General for the World Health Organization's Health Security
department, is
reported to have said:
"Without urgent, coordinated action by many stakeholders, the
world is headed for a post-antibiotic era… common infections and
minor injuries, which have been treatable for decades, can once
again kill."
Bacteria are intelligent enough to
outwit antibiotics through various means, as the study "The
Antibiotic Resistance Crisis"
mentions:
"In
bacteria, genes can be inherited from relatives or can be
acquired from nonrelatives on mobile genetic elements such as
plasmids.
This
horizontal gene transfer (HGT) can allow antibiotic resistance
to be transferred among different species of
bacteria. Resistance can also occur spontaneously through
mutation.
Antibiotics remove drug-sensitive competitors, leaving resistant
bacteria behind to reproduce as a result of natural selection."

Cannabis:
defeats cancer,
antibiotic-resistant bacteria and more!
Meet the Plant that Can Defeat
Some Strains of Antibiotic-Resistant Bacteria
Although Nature (and Man) has created a
problem, Nature has also created a solution.
It turns out that there may be an answer
to the problem of antibiotic overuse and antibiotic-resistant
bacteria:
cannabis.
Although it was demonized in the
1930s-1950s because of its threat to the oil, timber, clothing, fuel
and pharmaceutical industries, the scientifically proven truth has
emerged that cannabis (aka marijuana, hemp, weed or pot) has amazing
medical properties that we are just beginning to understand.
In an earlier article Cannabidiol
(CBD) - The Cat's Out of the Bag with This Cure-All, I
highlighted how just 1 cannabinoid out of more than 100 (namely
cannabidiol or CBD) was responsible for so many wonderful and
astounding health benefits, such as being anti-carcinogenic, neuro-protective,
anti-psychotic and anti-inflammatory.
Well, now you can add another great
medical property to the list: anti-bacterial or anti-microbial, and
not just against any ordinary bacterium.
A 2008 study entitled Antibacterial
Cannabinoids from Cannabis sativa - A Structure-Activity Study found
that cannabinoids have powerful anti-bacterial ability, including
against
MRSA:
"All
five major cannabinoids (cannabidiol, cannabichromene,
cannabigerol, Δ9-tetrahydrocannabinol, and cannabinol) showed
potent activity against a variety of methicillin-resistant Staphylococcus
aureus (MRSA) strains of current clinical relevance."
"All
compounds showed potent antibacterial activity… Activity was
exceptional against some of these strains, in particular the
multidrug-resistant (MDR) SA-1199B, which has a high level of
resistance to certain fluoroquinolones.
Also
noteworthy is the potent activity demonstrated against EMRSA-15
and EMRSA-16, the major epidemic methicillin-resistant S. aureus strains
occurring in U.K. hospitals.
These
activities compare highly favorably with the standard
antibiotics for these strains."
Conclusion - The Cannabis Plant is
a Highly Evolved Organism
The authors of the study state that,
"everything points towards these compounds having been evolved
by the plants as antimicrobial defenses that specifically target
bacterial cells",
...which suggests that we need to find
the answer to our problems in Nature, not in a laboratory, and
further reinforces the idea that plants are incredible organisms
upon which the literal survival of mankind depends.
Clearly,
the cannabis plant is a highly
evolved organism if it has developed
phytochemicals that can outwit
and defeat antibiotic-resistant bacteria and the most virulent of
superbugs.
The authors conclude:
"Given the availability of C. sativa strains producing high
concentrations of nonpsychotropic cannabinoids, this plant
represents an interesting source of antibacterial agents to
address the problem of multidrug resistance in MRSA and other
pathogenic bacteria.
This
issue has enormous clinical implications, since MRSA is
spreading throughout the world and, in the United States,
currently accounts for more deaths each year than AIDS."
What better proof could there be of the
utter backwardness of our world that marijuana is still classified
by the US Government as a Schedule 1 drug (meaning it has "no
currently accepted medical use" and "high potential for abuse"), yet
it may hold the key for unwinding the devastating harm done to the
world
by Big Pharma and its antibiotic overuse?
Sources
|